Skin Cancer: A Danger that is More than Skin Deep
Skin cancer is the most widespread form of cancer in the world. A skin cancer is diagnosed every 10 seconds in the United States. More people are diagnosed with skin cancer than all the other kinds of cancers combined. Incidents of skin cancer are on the rise. In 2012, the number of skin cancer diagnoses was approximately 3.4 million1. According to the American Cancer Society, there will be roughly 5.6 million cases diagnosed this year, an increase of almost thirty-seven percent2, 3. The majority of cases diagnosed were either basal or squamous cell carcinomas. Although basal cell carcinoma and squamous cell carcinoma are not inherently life-threatening, these tumors can be both painful and disfiguring. If left untreated, these tumor cells can mutate into more dangerous forms of cancer. These advanced forms can spread into other parts of the body and become deadly. In the United States alone, approximately 25,300 people die of skin cancer-related disease every year or one death about every hour.
Deaths associated with skin cancer are tragic because most cases are preventable with simple precautionary steps. In circumstances where skin cancer was not avoidable, many cases could have been successfully treated if immediate treatment was initiated with the discovery of the skin abnormality or lesion. In fact, if melanoma, one of the most deadly forms of skin cancer, is detected and treated promptly, the survivors have a ninety-eight percent survival rate. If melanoma goes untreated long enough to allow it to metastasize to other bodily systems, the survival rate decreases to twenty-three percent4.
What is Skin Cancer?
The body is comprised of trillions of cells. Each cell contains a complete strand of DNA which has around 20,500 genes within its code. The life cycle of the cell replicates by dividing into two identical halves in a process called mitosis.
When cells are damaged on a genetic level, their DNA mutates them into a form that is harmful to the body. This is how cancer cells are formed. When these cancers replicate and replace the healthy cells, they form large clumps known as a mass or tumor.
Many contributing factors can lead to the formation of cancer. Any external factor that significantly increases the likelihood that someone will develop cancer is called a carcinogen. The carcinogen that has the most significant influence on someone developing skin cancer is ultraviolet (UV) radiation. The UV radiation from direct sunlight exposure or tanning beds is linked to most of the cases of skin cancer. This is why most skin cancers typically arise on the more sun-exposed areas of the body like the face, chest, arms, legs, hands, ears, lips, and neck. Avid sun tanners may see skin cancer present itself in less exposed areas as well.
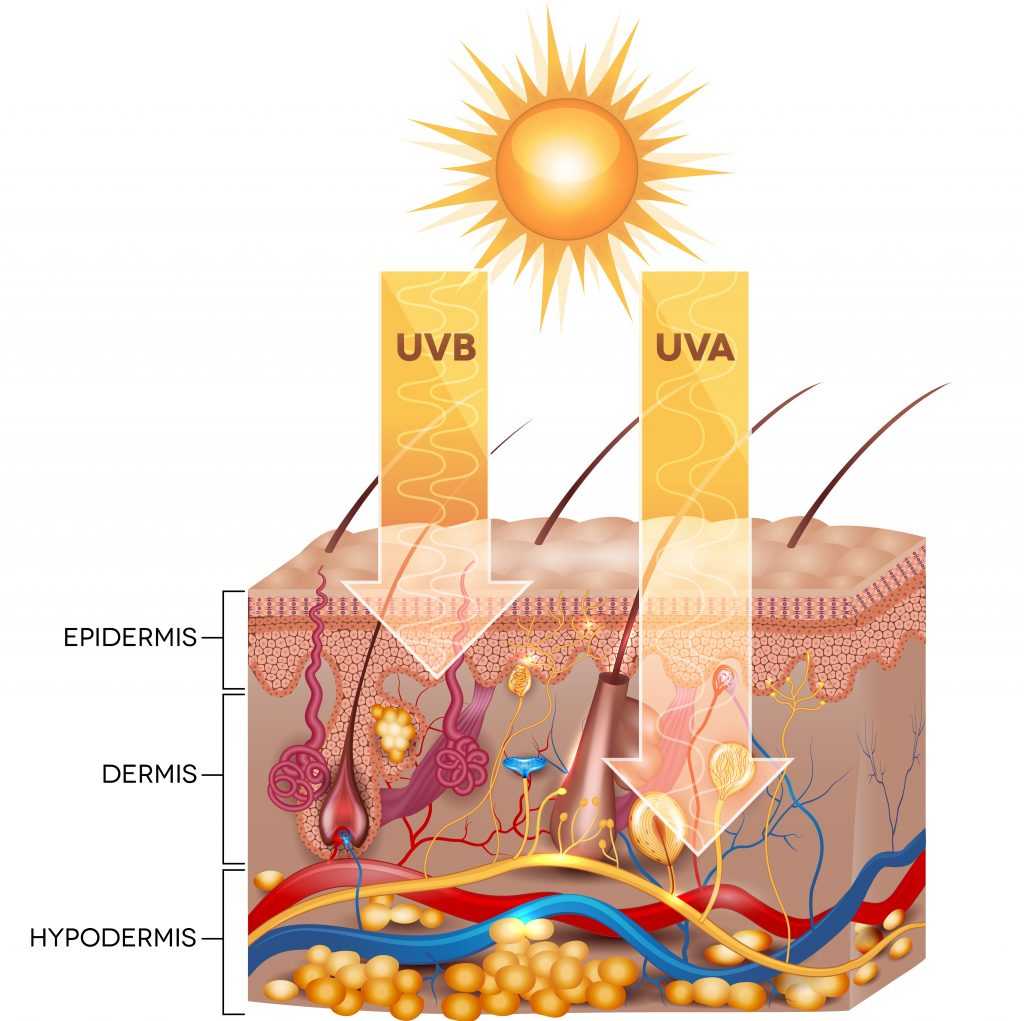
What are the Most Common Types of Skin Cancer?
A person’s visual symptoms can vary in presentation, depending on the kind of skin cancer they have. In the list below, we have a few more of the more common forms of skin cancer that Epiphany Dermatology treats.
Basal Cell Carcinoma5 is the most common form of cancer in the world. The basal cells, located at the bottom of the epidermal layer or topmost layer of the skin, are responsible for producing new skin cells when the old cells die off. Someone develops basal cell carcinoma after UV Rays mutate their basal cells. This typically happens in more sun-exposed areas of the skin, like the head or neck. Basal cell carcinoma can appear as the following presentations:
- A bump on the skin that can be white, flesh-toned, or pink
- A darker-colored lesion with a raised border
- A scaly, red-colored area
- A light-colored, wax-like scar
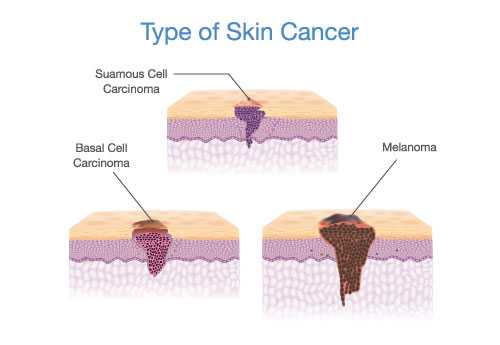
Squamous Cell Carcinoma6 is the second most widespread form of cancer. Squamous cells are within other structures of the body’s system and can be involved with different kinds of cancer. However, the squamous cells we are referring to in this article are the type of epithelial cells located in the skin’s epidermal layer of the skin. These cells are tightly packed together and serve as a barrier of the skin. As with most other cancers, when someone develops squamous cell carcinoma, it is usually secondary to exposure to UV radiation that causes their cell’s DNA to mutate. Typically, older skin cells are pushed to the surface of the epidermal layer for them to die and slough off naturally. When someone develops squamous cell carcinoma, this natural process is interrupted, causing the cells to reproduce at an exponential rate. Although squamous cell carcinoma is not inherently life-threatening, it is possible for it metastasize into other bodily systems and become dangerous to a patient’s health. Squamous cell carcinoma usually appears on the face, lips, ear, neck, and hands. People with darker skin tones are more likely to develop in areas of the skin that do not get as much UV exposure. Squamous cell carcinoma can appear as the following presentations:
- A red nodule
- An open sore or ulcer
- A crusty flaking sore that bleeds easily
Melanoma7 is considered one of the most severe and life-threatening forms of skin cancer. This kind of skin cancer forms in the melanocytes, the cells that are responsible for producing melanin or skin pigmentation. As with the other skin cancers, melanoma is strongly linked with exposure to UV radiation, but it can appear in places that haven’t had very much UV exposure. Melanoma most often develops on the face, chest, back, and legs. Individuals that have darker skin tones tend to form melanoma on their palms, soles of their feet, and under their nailbeds. Those with moles on their skin have to pay close attention to them. If their mole is asymmetrical, unusually colored, has irregular borders, larger than a ¼ inch, or evolving, they should seek immediate evaluation by a dermatologist. Since melanoma involves melanocytes, it generally appears as a darker area of skin. Melanoma cells grow at an accelerated rate and quickly crowd out the normal healthy cells, and have a propensity to metastasize or move to another system in the body, spreading the cancer. This is particularly dangerous for a patient if it metastasizes to the lymph node system. Some of the more common physical symptoms of melanoma are the following:
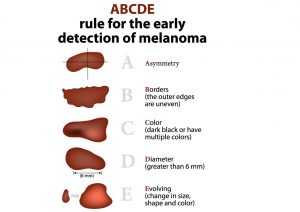
- Abnormal looking moles that are larger, asymmetric, irregularly bordered, unusually colored, and evolving in size, color and texture
- A large brown spot on the skin with usual markings
- The formation of an unusually pigmented area on the skin
- A discolored lesion with irregular borders that may or may not be painful to the touch
- Lesions that form on the palms of the hands, soles of the feet, nailbeds, mouth, nose, anus, or vagina
Actinic Keratosis (AK)8 is a coarse area of skin that usually develops after years of prolonged exposure to ultraviolet radiation. They typically grow on the head, face, neck, arms, and hands. Other than an odd patch of rough skin, actinic keratosis has no other signs or symptoms. Actinic keratosis are a precursor to skin cancers. Their typical presentation looks like the following symptoms:
- A rough, discolored patch of skin
- A bump that resembles a wart
What are the Risk Factors for Skin Cancer?
Skin cancer, like other forms of cancer, does not discriminate against who develops it. Certain risk factors will increase their vulnerability. These are a few of the more frequent risk factors:
Overexposure to sunlight – The sun’s ultraviolet radiation is one of the most prevalent carcinogens for skin cancer. People who have an active outdoor lifestyle that does not heed necessary precautions like seeking shade, avoiding the sun’s peak hours, and regular sunscreen application are at increased risk of developing skin cancer.
History of Sunburns – Building on the previous risk factor, a person with a history of at least five sunburns in their lifetime increases their risk of cancer by over 80 percent9. For this reason, people of this risk factor should use a sunscreen with a protection factor (SPF) of a minimum of 30, year around.
Tanning Bed Use – Some people want to improve their skin’s visual aesthetic by tanning. While laying out in the sun to achieve a more bronzed look has its own inherent risk, it is even more hazardous to use a tanning bed. The lamps in tanning beds project concentrated UVA and UVB rays into the skin. Over 419,000 cases of skin cancer a year have been linked to tanning bed use10. It is so prevalent that the United States Food and Drug Administration reclassified tanning beds as a class 2 risk device, meaning that they have a moderate to high risk of use11. In fact, 13 countries, 44 states, and the District of Columbia have either an outright band or placed restrictions on tanning bed use for anyone under the age of 181213. For their unprecedented correlation with skin cancer, the medical staff at Epiphany Dermatology strongly discourage the use of tanning beds for any reason.
Use of Tanning Oils – People should be using sunscreen year-round to prevent cellular damage of the UV Rays. This does not include the use of tanning oils of any kind. Epiphany Dermatology recommends a sunscreen of a minimum of SPF 30. Most tanning oils do not have any sunblock in their formulas, and those that do, usually have a protection factor of 15 if not a ridiculous 4 to 8. This is insufficient protection. Also, tanning oils FOCUS ultraviolet rays into the skin instead of repelling it like sunscreen14. By focusing the carcinogenic UV rays into the skin, tanning oils increases the risk of cellular sun damage and therefore, increase a person’s risk of skin cancer.
Fair Skin Tones – Although people of all skin tones can develop skin cancer, people of lighter skin tones are more susceptible. Melanin, the skin pigmentation produced by melanocytes, acts as a barrier to some UV radiation15. Therefore people of fairer skin tones whose bodies cannot produce as much melanin are more vulnerable to being damaged by UV rays, increasing their risk of skin cancer.
Family History – No other pre-existing condition is a higher predictor for skin cancer than a positive family history of cancer. If a person’s blood relatives have previously had skin cancer, then they should take extra precautions to ensure that they do not share their loved one’s fate.
Suppressed Immune System – Ultraviolet radiation is in itself an immunosuppressant, or stimuli that reduces the overall strength of the body’s natural defenses. A person with a lower immune system from their physical ailments, post-transplant surgeries, or immunosuppressive surgeries, etc. are at are at an increased risk for contracting skin cancer.
How Does Epiphany Dermatology Detect & Manage Skin Cancer?
Everything we do at Epiphany Dermatology is oriented to improve the health of our patients’ skin. Healthier skin leads to a healthier body. We are dedicated to our primary mission, the eradication of skin cancer. Better skin for a better life® drives our decision making.
FULL SKIN EXAM– Given that time is quality of life when it comes to detecting and treating skin cancer, annual full skin exams are crucial. The dermatologist performs a full skin inspection and discusses their finding with you, to come up with an individualized care plan to treat your skincare concerns. Sometimes during the exam, a biopsy is performed. The skin is removed and sent for evaluation by a doctor who specializes in looking at skin under the microscope.
VISIA Skin Analysis System– The skin on the face is one of the most common areas to form skin cancer. The VISIA Skin Analysis System is a comprehensive diagnostic tool that scans the face in no less than eight different settings. It’s in-depth evaluation looks for troublesome areas. It can spot anything from acne to melanoma. At least three of its diagnostic settings specifically look for the growth of skin cancer.
Photodynamic Therapy– In the event, that an actinic keratosis is discovered, the dermatologist can swiftly and effectively treat it with photodynamic light therapy. This treatment regimen can eradicate actinic keratosis before it can transform into squamous cell carcinoma.
Mohs Surgery– One of the most effective treatments for skin cancers like squamous cell carcinoma and basal cell carcinoma is Mohs Surgery. This procedure is performed at both Epiphany Dermatology’s Riverside and St. Joseph’s locations.
What are Some Other Resources to Help Avoid Getting Skin Cancer?
The majority of the cases of skin cancer are triggered by overexposure to UV radiation. When it comes to treating skin cancer, an ounce of prevention is truly worth a pound of cure. Below are listed a series of tips to help you enjoy your life and evade a potentially heartbreaking diagnosis of skin cancer.
Sunscreen – Sunscreen application should be a part of everyone’s daily skincare regimen. Everyone should use an SPF or protection factor of a minimum of 30. For people with fairer skin tones, they should consider a higher protection factor like SPF 50 and higher. Although some people are more mindful of sunscreen, during the hotter summer months, but not nearly enough people apply sunscreen during the colder winter months when sun damage is also prevalent. For dermatologist approved sunscreen click the link on the title.
Avoid Peak Hours of Sunlight – Between the hours of 10 a.m. and 2 p.m., the sun rays are at their strongest. This is particularly important during the summer time. Avoiding direct sunlight during these times can go a long way to prevent sun damage.
Sun Protective Clothing – The ability to wear sunscreen in the form of clothing is a wonderful option for kids and adults. These products have UPF which is similar to SPF. However, it does not change when it gets wet ie. the swim shirt. These can be an easy way to prevent sunburn and over exposure while still staying cool and comfortable. These products come in polyester and cotton. These include hats, swim suits, swim shirts, swim gloves and swim pants.
Seek Shade – Avoid sun damage by interspersing your outdoor activities with breaks in the shade.
Know your UV Index – The UV index indicates how strong the ultraviolet rays are in a particular area. Since UV rays are the chief carcinogenic that causes skin cancer, it’s vitally important to be aware of your local UV index when planning your daily activities. Fortunately, there are plenty of resources to find out what your current UV index is for your location. You can click the EPA widget below to find out your current UV index.
Eclipse Rx – Produced by Epiphany Dermatology’s own Dr. Brian Matthys, as a way to combat the growing epidemic of skin cancer. This wearable, water-resistant device keeps track of your time in the sun and links to an app on your smart phone to give you real-time feedback of your amount time in the sun. It reminds you to seek shade and when to reapply sunscreen. For more information on this life-changing product, please click the link the in the subheading.
For even more tips to help circumvent the dangers of the sun’s UV rays, we recommend this article about Ten Sun Smart Tips.
1 The American Cancer Society. (2012). Estimated New Cancer Cases and Deaths by Sex, US, 2012. Retrieved from https://www.cancer.org:
https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2012/estimated-number-of-new-cancer-cases-and-deaths-by-sex-2012.pdf
2 American Cancer Society. (2019). Cancer Facts & Figures 2019. Retrieved from https://www.cancer.org:
https://www.cancer.org/research/cancer-facts-statistics/all-cancer-facts-figures/cancer-facts-figures-2019.html
3 The American Society of Clinical Oncology. (2019, January). Skin Cancer (Non-Melanoma): Statistics. Retrieved from https://www.cancer.net:
https://www.cancer.net/cancer-types/skin-cancer-non-melanoma/statistics
4 The American Cancer Society medical and editorial content team. (2019, February 1). Survival Rates for Melanoma Skin Cancer. Retrieved from https://www.cancer.org:
https://www.cancer.org/cancer/melanoma-skin-cancer/detection-diagnosis-staging/survival-rates-for-melanoma-skin-cancer-by-stage.html
5 Mayo Clinic Staff. (n.d.). Squamous cell carcinoma of the skin. Retrieved from https://www.mayoclinic.org:
https://www.mayoclinic.org/diseases-conditions/squamous-cell-carcinoma/symptoms-causes/syc-20352480
6 Mayo Clinic Staff. (n.d.). Basal cell carcinoma. Retrieved from https://www.mayoclinic.org:
https://www.mayoclinic.org/diseases-conditions/basal-cell-carcinoma/symptoms-causes/syc-20354187
7 Mayo Clinic Staff. (n.d.). Melanoma. Retrieved from https://www.mayoclinic.org:
https://www.mayoclinic.org/diseases-conditions/melanoma/symptoms-causes/syc-20374884;l
8 Mayo Clinic Staff. (n.d.). Actinic Keratosis. Retrieved from https://www.mayoclinic.org:
https://www.mayoclinic.org/diseases-conditions/actinic-keratosis/symptoms-causes/syc-20354969
9 Deborah S. Sarnoff, M. (2015, July 15). The Skin Cancer Foundation’s Official Position on Sunburn Art. Retrieved from https://www.skincancer.org:
https://www.skincancer.org/media-and-press/press-release-2015/sunburns
10 Wehner MR, C. M. (2014, May). International prevalence of indoor tanning: a systematic review and meta-analysis. Retrieved from https://www.ncbi.nlm.nih.gov:
https://www.ncbi.nlm.nih.gov/pubmed/24477278
11 NCI Staff. (2014, July 24). U.S. Indoor Tanning Rates Are Dropping, But Still High. Retrieved from https://www.cancer.gov:
https://www.cancer.gov/news-events/cancer-currents-blog/2015/indoor-tanning
12 Staff of NCSL. (2018, November 2). Indoor Tanning Restrictions for Minors | A State-By-State Comparison. Retrieved from http://www.ncsl.org:
http://www.ncsl.org/research/health/indoor-tanning-restrictions.aspx
13 The Skin Cancer Foundation. (2019, April 27). Skin Cancer Facts & Statistics. Retrieved from https://www.skincancer.org:
https://www.skincancer.org/skin-cancer-information/skin-cancer-facts
14 Sherwood, C. (n.d.). How Tanning Oil Works. Retrieved from https://www.livestrong.com:
https://www.livestrong.com/article/71789-tanning-oil-works/
15 Health Engine. (2006, March 3). Skin Colour. Retrieved from https://healthengine.com.au:
https://healthengine.com.au/info/skin-colour
To find out more about Skin Cancer Treatments at Epiphany Dermatology – Kansas City
Our Riverside Location:
805 NW Platte Rd., Suite 120
Riverside, MO 64150 | CLICK HERE for Directions
Phone: (816) 205-8120
SEND US AN E-MAIL
Our St. Joseph Location:
805 N 36th St., Suite D
St. Joseph, MO 64506 | CLICK HERE for Directions
Phone: (816) 205-8120
SEND US AN E-MAIL

